
According to the “Huangdi Neijing (Yellow Emperor’s Inner Canon) – Suwen (Basic Questions) – Chapter on the Five Qi”: “The five organs transform into fluids: the heart produces sweat, the lungs produce mucus, the liver produces tears, the spleen produces saliva, and the kidneys produce spittle; these are known as the five fluids.“
When food enters the stomach, its essence transforms into fluids, which are stored in the five organs. When the five organs are filled with fluids, they can be distributed to the external orifices, resulting in sweat, mucus, tears, saliva, and spittle, which are referred to as the five fluids. The “five fluids” are components of the body’s normal water and fluids, formed by the fluids of the five organs being filled and distributed to the external orifices.
 Tears as the Fluid of the Liver
Tears as the Fluid of the Liver
In Traditional Chinese Medicine (TCM), tears are considered to be transformed from the essence and blood of the liver. The liver opens to the eyes, and tears flow from the eyes, hence the saying “tears are the fluid of the liver.” Tears serve to moisten and protect the eyes.
The Liver and Tears
Under normal circumstances, the secretion of tears is moistening and not overflowing; however, when foreign objects invade the eyes, tears can be secreted in large amounts to cleanse the eyes and expel foreign matter.
In pathological conditions, abnormal secretion of tears can be observed. For instance, insufficient liver blood can lead to reduced tear secretion, commonly resulting in dry eyes; conditions such as wind-heat conjunctivitis and damp-heat in the liver channel can lead to increased eye discharge and tears flowing in the wind.
Additionally, in cases of extreme sorrow, the secretion of tears can also increase significantly.

Long-term excessive eye use and staying up late can deplete liver blood, leading to insufficient liver blood and the rise of false fire, resulting in a series of symptoms of insufficient tear secretion such as dry and itchy eyes.
Recommendations for Care
1. Avoid excessive eye use: Be conscious of blinking more often, and after using electronic devices for about 40 minutes, move the eyes up, down, left, and right to exercise them.
2. Warm compresses before bed: This can improve blood circulation around the eyes and enhance the secretion of meibomian glands, alleviating dry eye symptoms.
3. Reduce the use of eye drops: Long-term use of certain eye medications may lead to dry eye syndrome.
 Sweat as the Fluid of the Heart
Sweat as the Fluid of the Heart
Sweat is the fluid that is expelled from the body through the sweat pores after the evaporation of fluids by yang energy. The “Suwen – Theory of Yin and Yang” states: “Yang added to Yin is called sweat.”
The heart is associated with sweat, indicating that heart blood and heart essence are the source of sweat production. The “Suwen – Theory of the Generation of the Five Organs” states, “The five organs transform into fluids; the heart produces sweat.”
The Heart and Sweat
The generation and excretion of sweat are closely related to heart blood and spirit. The heart governs the blood vessels, and blood and fluids share a common source and transform into each other. When the water in the blood seeps out of the vessels, it becomes fluids, which are the source of sweat production. When the heart blood is abundant and the fluids are sufficient, sweat can be produced to nourish the skin and expel waste from the body.
The heart also houses the spirit, and the generation and excretion of sweat are governed and regulated by the heart spirit. When the heart spirit is clear, it responds sensitively to various internal and external information, and the generation and excretion of sweat will adjust accordingly to physiological conditions and external climate changes. Therefore, sweating can be observed during emotional tension, excitement, labor, exercise, and hot weather.
Generally, sweating is a normal physiological phenomenon that protects the body. Through sweating, the body can expel excess moisture and dispel heat, achieving a balance of yin and yang.
For instance, in hot weather, during intense activity, or after drinking hot water or consuming spicy food, the sweat pores will open, and sweating will increase to timely release heat and protect the body. Conversely, when it is cold, drinking cold beverages, and resting at night, the sweat pores will close, and sweating will decrease to avoid damaging yang energy.
However, it is important to note that excessive sweating can deplete heart energy or heart yang, and profuse sweating can lead to a critical condition of heart energy or heart yang collapse.

In TCM, if one sweats frequently during the day, especially with slight activity, it is called spontaneous sweating, often caused by spleen and lung qi deficiency, commonly presenting as shortness of breath, fatigue, susceptibility to colds, pale complexion, or accompanied by chills.
If sweating occurs during sleep and stops upon waking, even soaking the clothes and bedding, it is called night sweats, often due to yin deficiency. This is commonly accompanied by heat in the palms and soles, dry mouth and throat, insomnia, and flushed cheeks.
Recommendations for Care
1. Dietary care: For qi deficiency spontaneous sweating, it is advisable to frequently consume foods that tonify qi and stabilize the exterior, such as honey, yam, jujube, and astragalus. For yin deficiency night sweats, it is advisable to consume foods that nourish yin and tonify the kidneys, such as pig kidneys, duck meat, black beans, and goji berries.
2. Acupoint massage: Hegu (LI4) and Fuliu (KD7) are commonly used acupoints to stop sweating, effective for both spontaneous sweating and night sweats.
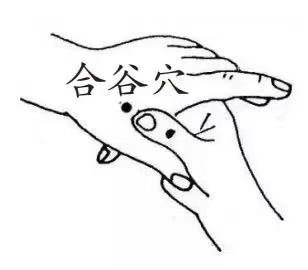
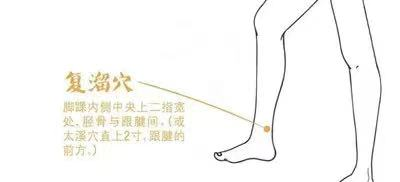
3. Herbal tea care: Use 6 red dates and 10 grams of astragalus, add an appropriate amount of water, and boil to make a tea that can tonify qi and stabilize the exterior, suitable for qi deficiency spontaneous sweating.
 Spittle as the Fluid of the Kidneys, Saliva as the Fluid of the Spleen
Spittle as the Fluid of the Kidneys, Saliva as the Fluid of the Spleen
Spittle, is the thicker part of saliva, primarily secreted from under the tongue, serving to moisten the mouth, lubricate food, and nourish kidney essence.
Saliva, is the thinner part of saliva, produced by the essence and qi of the spleen, thus it is said that “the spleen produces saliva.”
The Kidneys and Spittle
Spittle is produced from kidney essence, propelled by kidney qi, traveling along the foot shaoyin kidney channel, passing through the liver, diaphragm, lungs, and trachea, reaching the sublingual areas known as Jinjin and Yuye, where it is secreted. Thus, the “Suwen – Chapter on the Five Qi” states: “The five organs transform into fluids… the kidneys produce spittle.”
Since spittle originates from kidney essence, if swallowed and not spat out, it can nourish kidney essence; however, excessive spitting can deplete kidney essence. Therefore, ancient health practitioners advocated “swallowing spittle” to nourish kidney essence.
The Spleen and Saliva
Saliva protects the oral mucosa and moistens the mouth, being secreted abundantly during eating to assist in chewing and digestion, hence the saying “saliva is produced by the spleen and overflows into the stomach.”
Under normal circumstances, when the spleen’s essence and qi are sufficient, saliva is produced in appropriate amounts, rising to the mouth without overflowing. If the spleen and stomach are not harmonious, or if the spleen qi fails to contain, it can lead to abnormal excessive saliva production, resulting in saliva flowing from the mouth. If the spleen essence is insufficient, fluids are not abundant, or the spleen qi loses its ability to promote and stimulate, then saliva secretion may be low, leading to dry mouth and tongue.
Although spittle and saliva are both secretions from the mouth, they have distinct differences. Saliva is transformed from spleen essence, secreted from the cheeks, and is thinner, while spittle is produced from kidney essence, secreted from under the tongue, and is thicker, often spat out. Therefore, in clinical treatment, excessive saliva from the mouth is often treated from the spleen, while frequent spitting is treated from the kidneys.

TCM believes that saliva can “moisten the five organs, beautify the skin, strengthen teeth, strengthen bones, promote qi and blood circulation, and prolong life.”
During the Spring and Autumn period, Laozi believed that while elixirs are good, they are not as important as one’s own fluids. Ancient health practitioners like Tao Hongjing also stated: “Consuming the jade spring can prolong life and eliminate diseases.”
Saliva is transformed from the spleen and kidneys, with the kidneys being the source of innate essence and the spleen being the source of acquired essence. The spleen and stomach gather the essence of the five organs and the essence of qi and blood, thus saliva contains many beneficial substances for health and longevity, playing a special role in health preservation.
Ancient physicians believed that those with abundant saliva must have a strong constitution, and they assessed disease conditions based on the abundance or deficiency of saliva.
Recommendations for Care
1. Stay hydrated: When the mouth is dry and lacks fluids, drink water promptly.
2. Eat sour foods in moderation: Foods like hawthorn and plums that easily generate fluids can be consumed, but those with spleen and stomach diseases should eat less.
3. Regularly swallow saliva: Each morning, use the tip of the tongue to lick the upper palate, allowing saliva to gather in the mouth, and swallow it in several portions.
4. Frequently puff the cheeks: This action can help secrete a large amount of saliva and promote digestion.
 Mucus as the Fluid of the Lungs
Mucus as the Fluid of the Lungs
Mucus, or nasal mucus, is the secretion of the nasal mucosa, serving to moisten the nasal passages. Mucus is transformed from lung essence and is distributed to the nasal passages through the dispersing action of lung qi, hence the “Suwen – Chapter on the Five Qi” states: “The five organs transform into fluids… the lungs produce mucus.”
Under normal circumstances, mucus is colorless and transparent, serving to moisten the nasal passages, keeping them clear, and ensuring normal respiratory and olfactory functions.

The Lungs and Mucus
The condition of lung essence and lung qi can also be reflected in the changes of mucus. If lung essence and lung qi are sufficient, mucus will moisten the nasal passages without flowing out. If cold pathogens invade the lungs, lung qi will fail to disperse, and the lung fluids will be congealed by cold pathogens, leading to a runny nose; if there is lung heat, symptoms such as wheezing, coughing, and yellow mucus may occur; if dryness invades the lungs, it can lead to nasal dryness and pain.
In terms of colds, observing the color of mucus can help preliminarily determine whether it is due to wind-cold or wind-heat, allowing for appropriate treatment to alleviate cold symptoms.
When external cold pathogens harm the lungs, it can easily lead to wind-cold colds, resulting in a runny nose with cool, clear mucus; if it is a wind-heat cold, it will result in warm, yellow mucus.
Recommendations for Care
1. For wind-cold colds: In the early stages, take 150 grams of tofu and 6 grams of fermented soybeans, boil with 400 milliliters of water until reduced to 200 milliliters, then add 3 segments of green onion and boil again to drink. This dietary therapy has the effect of dispersing cold.
2. For wind-heat colds: In the early stages, use 3 grams each of mulberry leaves, chrysanthemum, mint, and淡竹叶 (Dan Zhu Ye – Lophatherum gracile) with an appropriate amount of honey, boil and drink as tea for three days. This formula has the effect of dispersing wind-heat.
Source: Guangdong Traditional Chinese Medicine. For further understanding of TCM diagnostic and treatment methods, please consult the TCM team at Qidong Fifth People’s Hospital.



Introduction to the TCM Team at Qidong Fifth People’s Hospital



Summer Wei Ming
Former Deputy Secretary and Vice President of Qidong Traditional Chinese Medicine Hospital, Chief TCM Physician, and Renowned TCM Physician in Nantong. Specializes in the treatment of spleen and stomach diseases, liver and kidney diseases, particularly chronic gastritis, precancerous lesions of gastric cancer, gastrointestinal tumors, ulcerative colitis, chronic hepatitis, liver cirrhosis, biliary diseases, migraines, chronic nephritis, renal function impairment, coronary heart disease, and other difficult diseases with unique experience in TCM treatment.

Peng Lei
Deputy Chief of Internal Medicine at Qidong Traditional Chinese Medicine Hospital, Associate Chief TCM Physician, graduated from Shanghai University of Traditional Chinese Medicine, studied under renowned TCM physician Sha Jianfei from Jiangsu Province. Has clinical experience in common and frequently occurring internal diseases, especially in the diagnosis and treatment of respiratory, digestive, and cardiovascular diseases.

Sha Hongbiao
Associate Chief Physician at Qidong Traditional Chinese Medicine Hospital, graduated from Nanjing University of Traditional Chinese Medicine (now Nanjing University of Chinese Medicine) with a specialization in acupuncture and tuina. Has in-depth research on the treatment of sequelae of stroke, cervical spondylosis, shoulder periarthritis, tennis elbow, tenosynovitis, acute and chronic low back pain, lumbar disc herniation, sciatica, facial paralysis, neurogenic headache, and common pediatric tuina diseases (such as colds and digestive disorders).

Qiu Nanbin
Director of the Medical Affairs Department (Doctor-Patient Relationship Department) at Qidong Fifth People’s Hospital, attending TCM physician, self-taught graduate of Nanjing University of Traditional Chinese Medicine. Has insights into chronic gastritis, bile reflux gastritis, liver and gallbladder diseases, neurasthenia, insomnia with night sweats, and the use of Chinese medicine to regulate sub-healthy constitutions.

Sun Feihu
Group Leader of the Medical Affairs Department (Doctor-Patient Relationship Department) at Qidong Fifth People’s Hospital, attending TCM physician, graduated from Nanjing University of Traditional Chinese Medicine. Has experience in treating internal diseases, auricular acupressure, and particularly in TCM treatment of cardiovascular diseases.

Liu Yong
Attending TCM physician and rehabilitation therapist at Qidong Fifth People’s Hospital, graduated from China Yangtze River Three Gorges Engineering School, continued education at Beijing University of Traditional Chinese Medicine. Specializes in acupuncture, small needle knife, and tuina for treating neck, shoulder, waist, and leg pain, tenosynovitis, migraines, facial nerve paralysis, sequelae of stroke, and joint mobility disorders after trauma.

Xue Dongqing
Assistant TCM physician at Qidong Fifth People’s Hospital, trained under the renowned TCM physician Chen Xiling (grandfather) and the famous TCM physician Xia Weiming from Nantong. Clinically adept at using pure TCM techniques to treat common diseases in internal medicine and gynecology, specializing in dysmenorrhea, irregular menstruation, menopausal syndrome, chronic pelvic inflammatory disease, spontaneous sweating, night sweats, urticaria, insomnia, dizziness, palpitations, migraines, tennis elbow, neck, shoulder, waist, and leg pain, and sciatica.
END
Editor | Wang Pengyun
Reviewed by | Qiu Hongxia


