Inquiry is crucial for treatment, as it allows for a quick understanding of the patient’s main complaints and helps form a mental picture of the possible causes of the symptoms. During the patient’s responses, relevant diagnostic and treatment thoughts can be formed. This article summarizes common inquiries related to patients with cervical spondylosis and their implications.
1. Patient’s Age
Note: Degenerative changes in the joints are common in individuals over 25 years old, with 60% of those over 45 years and 85% of those over 65 years showing such changes. Bone and joint issues are more prevalent in individuals over 60 years old.
Many imaging studies show no direct correlation with the patient’s symptoms.
2. Patient’s Symptoms
Note: The way patients express their symptoms helps the therapist understand the general condition of the patient and whether there is nerve compression in the cervical spine leading to lesions. What is the prognosis for the patient?
Differential diagnosis of cervical spondylosis, cervical spinal stenosis, and cervical disc herniation
|
Cervical Spondylosis |
Cervical Spinal Stenosis |
Cervical Disc Herniation |
|
|
Pain |
Usually unilateral pain |
Bilateral or unilateral pain |
Unilateral pain is more common or bilateral |
|
Pain Area |
Radiates to the surface |
Usually affects certain skin areas |
Radiates to the surface |
|
Pain on Extension |
Relieved |
Worsened |
May be relieved |
|
Pain on Flexion |
Worsened |
Relieved |
Worsened (common) or relieved |
|
Relief at Rest |
Yes |
Yes |
No |
|
Patient Age Group |
Gradually younger |
Common in ages 30-60 |
17-60 years |
|
Instability |
May exist |
Does not exist |
Does not exist |
|
Multiple Segments Affected |
C5/6, C6/7 |
Any segment may be affected |
C5/6 |
|
Onset |
Gradual |
Gradual (may complicate the other two) |
Sudden |
|
Imaging Examination |
Can confirm diagnosis |
Can confirm diagnosis |
Can confirm diagnosis (needs to be combined with clinical findings) |
3. What is the mechanism of injury?
Note: Is there any history of trauma, pulling, or overuse? Was the injury sustained during movement?
If the patient has been overusing or maintaining a posture for a long time, it may be upper cross syndrome or thoracic outlet syndrome; if there is a history of trauma, it may be a neck sprain caused by whiplash and related disorders.
4. What is the patient’s usual work or activity style?
Note: Are there specific activities or postures that cause discomfort? What is the patient’s occupation? Does it require maintaining a posture for long periods?
Pain at the cervicothoracic junction often arises from activities involving pushing and pulling, such as mowing, sawing, and cleaning windows.
5. Has there ever been a head impact or car accident?
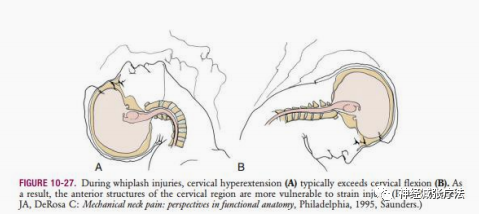
Note: If the injury is due to a car accident, consider whether the patient has whiplash injury, deep flexor muscle injury, leading to reduced cervical stability, resulting in a series of symptoms related to cervical instability.
For example: swallowing difficulties, recurrent stiff neck, etc.
6. When did the symptoms start?
Note: If it is post-trauma, bone pain occurs immediately, but muscle or ligament pain may be immediate (e.g., laceration) or may occur hours or days later (e.g., strain from a car accident). 70% of whiplash injury patients will have symptoms immediately, while others may have delayed onset. Myofascial pain often has three trigger points, and soreness may persist for more than 3 months without a clear history of trauma.
7. What is the location and extent of the pain?
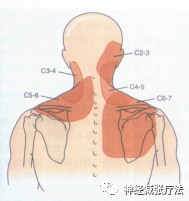
Note: Please have the patient indicate the location of the pain. Damage to the nerve roots at C4 and above will not affect the arms. Cervical radiculopathy or cervical nerve root injury primarily presents with unilateral upper limb motor and sensory symptoms, including weakness (myotome), sensory changes (dermatome), reduced reflexes, and limited local movement.
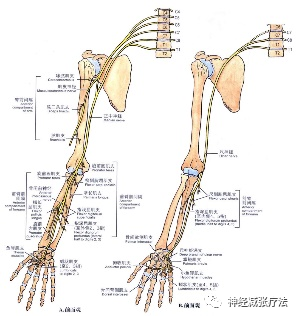
Cervical nerve compression often presents with symptoms radiating to the shoulder, scapula, and upper arm. Compression of the cervical spinal cord may lead to sensory abnormalities, unilateral or bilateral lower limb coordination issues, and dysfunction of proprioception or sphincter muscles.
8. Does the pain radiate?
Note: Is the pain deep? Radiating? Burning? Aching? For example, when an athlete feels a burning sensation, it feels like a lightning-like burning pain radiating to the shoulder and arm, followed by a feeling of heaviness or loss of sensation. Dysfunction of the cervical facet joints can lead to referred pain in the neck and shoulder area.
9. Does the pain get affected by laughing, coughing, sneezing, or straining?
Note: If so, it is due to increased pressure in the thoracic or abdominal cavity.
10. Does the patient experience headaches? If so, where? How often do they occur?
Note: If it is cervicogenic headache, the area of the headache can indicate the injured nerve area.
11. Does changing positions affect the headache or pain?
Note: If so, which positions increase or decrease the headache? The patient may describe pain and radiating symptoms that change with arm or head movements, worsening or alleviating; this phenomenon is called Bakody’s sign, usually indicating an issue at C4/5.
12. Are there any sensory abnormalities? (Tingling, burning sensations)
Note: Such sensations occur when the nerve roots are compressed. They may become more pronounced after the pressure on the nerve trunk is relieved, and numbness or sensory abnormalities in the hands or legs, as well as deterioration of hand function, may be related to cervical myelopathy.
Bilateral upper limb paresthesia often indicates systemic diseases (such as diabetes, excessive alcohol consumption) leading to neuropathy or spinal cord ischemia or space-occupying lesions in the spinal cord.
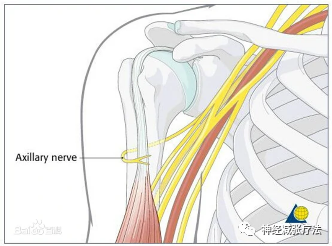
13. Are there any symptoms in the lower limbs?
Note: Such findings may indicate serious issues with the spinal cord. For instance, cervical myelopathy symptoms include numbness, sensory abnormalities, ataxia, difficulty walking, and lack of balance and agility. All these symptoms indicate cervical myelopathy. Additionally, sphincter (bowel or bladder) or sexual dysfunction may also be related to cervical myelopathy.
14. Does the patient have difficulty walking? Any balance issues?
Note: Is there a staggering gait? Or difficulty walking in the dark or an increased width of the stance? If so, it indicates a possible cervical spinal cord lesion. Abnormalities in cranial nerves combined with gait changes may indicate systemic neurological dysfunction.
15. Has the patient ever experienced dizziness, fainting, or seizures?
Note: What is the degree, frequency, and duration of dizziness? Is it related to specific head or body positions? Issues with the semicircular canals and vertebral arteries can cause dizziness. If a non-volitional fall occurs while the patient is conscious, it is called a sudden fall. Does the patient experience diplopia, nystagmus, etc., which may indicate serious injury, nerve damage, or sometimes increased intracranial pressure?
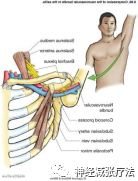
16. Does the patient report any symptoms related to the sympathetic nervous system?
Note: This may be due to damage to the soft tissues on the anterior and lateral sides of the neck, affecting the cranial nerves and sympathetic nerves passing below. Severe injuries (e.g., acceleration or whiplash injuries) can lead to sympathetic nervous system hyperactivity, with symptoms including tinnitus, dizziness, blurred vision, photophobia, rhinorrhea, sweating, tearing, and weakness.
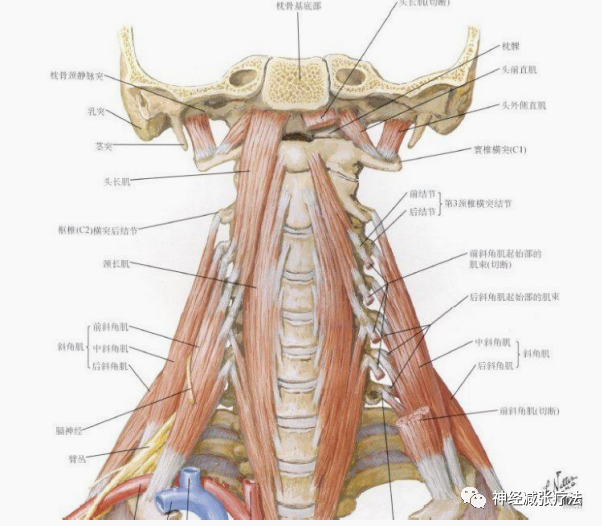
17. Has there been any improvement, worsening, or no change in the condition since the onset?
Note: This can help understand the progression of the patient’s condition and their prognosis.
18. What activities have led to worsening? What activities relieve symptoms?
Note: Are there any head or neck positions that exacerbate symptoms? These positions should be noted; for example, does it feel uncomfortable when the neck is bent? If the change in posture does not affect symptoms, the issue may not be musculoskeletal. Injuries at C3, C4, and C5 can affect the diaphragm, thus impacting breathing.
19. Does the patient have any limitations in activity?
Note: If so, which movements are limited? Assessing movements can help identify the site of the patient’s injury.
20. Are there any breathing issues?
Note: Breathing can be chest, abdominal, shoulder, or reverse breathing. The trapezius, scalene, and sternocleidomastoid muscles located in the neck are important accessory muscles for expiration; if these muscles are injured, it greatly affects breathing patterns.
Breathing is closely related to spinal stability; if the patient has breathing issues, there will certainly be problems with spinal stability, leading to pain.
21. Is there difficulty swallowing? Or any changes in voice?
Note: Such changes may be due to nerve issues, cervical positioning, or muscle incoordination. Swallowing difficulties may be related to swelling of the soft tissues in the pharynx, tension, cervical subluxation, bone spur protrusions, or disc herniation compressing the pharynx or esophagus. Additionally, swallowing may become difficult and the voice may weaken when the cervical spine is extended backward.
22. What is the patient’s sleeping position?
Note: Are there any sleep issues? Does the patient prefer sleeping on their side or back? Is there an issue with the height of the pillow?
Too high a pillow: When lying on the back, it can lead to a straightening of the cervical curve.
When sleeping on the side, the lower muscles may be overstretched and painful.
Too low a pillow: When sleeping on the side, the upper muscles may be overstretched.
Sleeping on the stomach is not advisable as it can cause neck rotation.
Currently, there are three offline training materials available: the first is on lumbar nerve decompression therapy, the second is on cervical upper limb issues, and the third is on peripheral nerve pathways, compression points, symptoms, etc. If interested, please contact us. After purchase, you will be added to a study group for Q&A and sharing.


